
A new healthcare invention from the University of Tennessee Health Science Center’s (UTHSC) Center for Healthcare Improvement and Patient Simulation (CHIPS) in Memphis is a true testament to scientific collaboration and the power of the University of Tennessee ecosystem.

In April 2019, a team of researchers and practitioners debuted an Infant Pericardiocentesis Trainer at the Patent Ductus Arteriosus (PDA) Symposium in Memphis. The team of inventors includes Jonathan Spagnoli, lead inventor and CHIPS simulation specialist; Jarrod Young, CHIPS simulation operations lead; Dr. Sandeep Chilakala, associate professor of pediatrics- neonatology; and Dr. Ranjit Raju Philip, assistant professor of pediatrics-cardiology.
“This whole process has been a true testament to collaboration,” said Ranjit. “That’s the advantage of an umbrella system like UT, which provides many opportunities to meet new people and collaborate. That has been the biggest success.”
The Infant Pericardiocentesis Trainer educates medical professionals in blind or ultrasound-guided infant pericardiocentesis. Pericardiocentesis is the definitive emergency treatment for tamponade, a life-threatening condition caused by fluid accumulation around the heart. The condition rarely occurs, yet when it does, the procedure must be conducted accurately within a matter of minutes. Due to the rarity of the condition, physicians with limited exposure to it might spend much of their career lacking the knowledge or skill needed to perform this life-saving procedure.
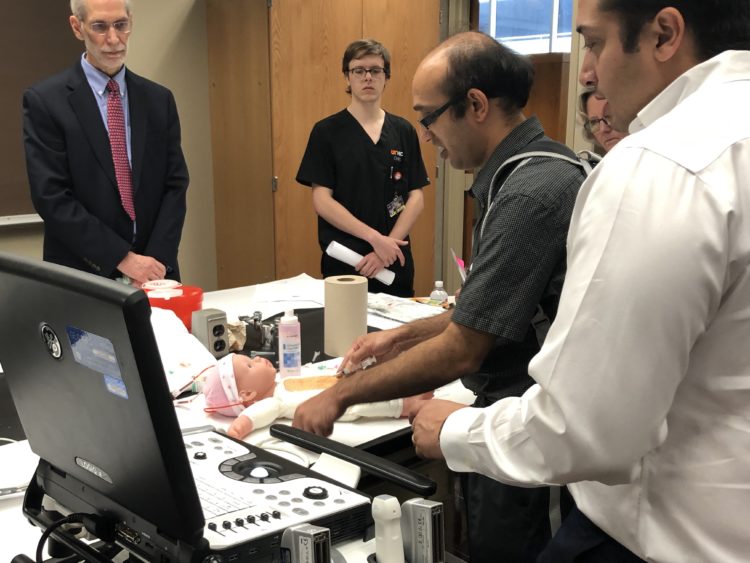
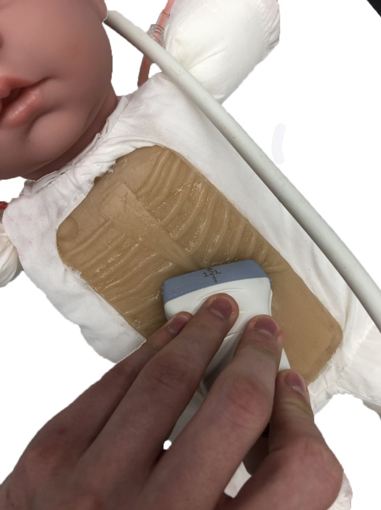
Jonathan and the team designed the trainer (which is placed in a baby doll to increase the realistic nature of the simulation) with ultrasound-capable tissue that allows for the option of blind or guided access into the pericardium, the outside membrane of the heart. To make the trainer even more realistic, it features dual chambers with separate fluid ports and colors that provide visual feedback for the trainee. Essentially, if a trainee inserts the needle too far, they would see a different color.
“There’s a growing awareness in the field of healthcare simulation now that doing something once doesn’t mean mastery,” Jarrod explained. “Continual training and refining skills help you continue that skill long term. This trainer would be available for every practicing physician to help prepare them to offer the best set of skills to any patient that they see.”
Another vital part of the collaborative process has been UTRF. Chad Epps, executive director of healthcare simulation at CHIPS, urged the team to go to UTRF to explore if the trainer was patentable. Without the organization’s support, Jonathan remarked that the technology would not be where it is today.
“UTRF showed us the potential we didn’t know our technology had,” Jonathan said. With UTRF’s guidance, Jonathan and the team attended UT Day on the Hill, meeting with state legislators and gaining valuable connections and visibility. The latest Memphis Scipreneur Challenge also featured the technology.
Regarding next steps, the team would like to see the trainer distributed as widely as possible at an affordable cost to improve patient safety because, as Jonathan mentioned, the more physicians and institutions who have access to it, the better. Sandeep elaborates, “In addition to medical students and residents, this would not only be invaluable training to over 8,000 practicing neonatologists but also to ER physicians and pediatric intensivists.”
With the help of UTRF, the team is currently looking for commercialization partners. In October, they plan to bring more trainers to the PDA Symposium 2020 in Las Vegas. Additionally, all new pediatric cardiology fellows at UTHSC that begin this summer will practice with the trainer as part of their initial simulation training.
“UTRF is dedicated to helping healthcare technology, like the Infant Pericardiocentesis Trainer, reach its fullest potential,” remarked UTRF Licensing Associate Dr. Delira Robbins. “We are excited to witness the next stage of this journey and believe this trainer has the potential to make a real, lasting impact for practitioners in the field.”